For many people, glasses and contact lenses are part of everyday life. While these solutions effectively correct vision, some patients prefer a more permanent option that reduces or eliminates dependence on corrective lenses.
In recent years, refractive surgery has become increasingly popular as technology continues to improve the safety and precision of vision correction procedures. Modern techniques allow ophthalmologists to correct common vision problems while offering relatively quick recovery times.
Understanding the different refractive surgery options available can help patients decide whether surgical vision correction is suitable for their needs.`
What Is Refractive Surgery?
Refractive surgery refers to procedures that correct vision by changing how light is focused within the eye.
Definition and goal
The goal of refractive surgery is to improve visual clarity by adjusting the eye’s focusing ability. This is usually achieved by reshaping the cornea or replacing the natural lens of the eye.
By improving how light reaches the retina, these procedures can reduce or eliminate the need for glasses or contact lenses.
Common vision problems it addresses
Refractive surgery is commonly used to treat:
- Myopia (short-sightedness)
- Hyperopia (long-sightedness)
- Astigmatism
- Presbyopia
Different procedures are designed to address different visual needs, which is why a personalised evaluation is necessary before treatment.
Importance of personalised assessment
Not every patient is suitable for every procedure. Factors such as age, corneal thickness, eye health, and lifestyle all influence which refractive surgery option may be most appropriate.
A comprehensive eye examination helps determine whether surgery is suitable and which procedure may offer the best outcome.
LASIK: How It Works and Who It Suits
LASIK is one of the most widely performed forms of refractive surgery worldwide.
Procedure overview
During LASIK surgery:
- A thin flap is created on the surface of the cornea.
- A laser reshapes the underlying corneal tissue.
- The flap is repositioned to allow the eye to heal naturally.
The reshaping process helps light focus more accurately on the retina.
Ideal candidates
LASIK may be suitable for patients who:
- Have stable vision prescriptions
- Have sufficient corneal thickness
- Do not have significant eye surface conditions
- Wish to reduce dependence on glasses or contact lenses
Key benefits and limitations
Benefits may include:
- Rapid visual improvement
- Short procedure time
- High success rates for many patients
Potential limitations include:
- Not suitable for very thin corneas
- Some patients may experience temporary dry eyes
- Vision may still change gradually with age
Typical recovery timeline
Most patients notice improved vision within 24 to 48 hours after LASIK. Many can resume normal activities within a few days, although full stabilisation may take several weeks.
SMILE: Key Differences and Benefits
SMILE (Small Incision Lenticule Extraction) is a newer type of laser refractive surgery designed to treat myopia and astigmatism.
How SMILE differs from LASIK
Unlike LASIK, SMILE does not require the creation of a corneal flap. Instead, the laser creates a small lens-shaped piece of tissue within the cornea, which is then removed through a tiny incision.
Because the procedure involves a smaller incision, it is considered a minimally invasive technique.
Suitable patient profiles
SMILE may be suitable for patients who:
- Have myopia or myopia with astigmatism
- Prefer a flap-free procedure
- Lead active lifestyles or participate in contact sports
Advantages for active lifestyles and dry-eye concerns
Some patients prefer SMILE because:
- It preserves more corneal structure
- It may reduce the risk of flap-related complications
- It may be associated with fewer dry-eye symptoms in some cases
Recovery expectations
Vision improvement is usually noticeable within a few days. Most patients return to daily activities relatively quickly, although full visual stability may take a few weeks.
Clear Lens Extraction (CLE): When It’s Recommended
Clear Lens Extraction (CLE) is another form of refractive surgery that involves replacing the eye’s natural lens.
What CLE involves
During CLE, the natural lens of the eye is removed and replaced with an artificial intraocular lens (IOL), similar to the procedure performed in cataract surgery.
The artificial lens is selected to correct refractive errors and improve visual clarity.
How it differs from laser procedures
Unlike LASIK or SMILE, CLE does not reshape the cornea. Instead, it changes the eye’s focusing ability by replacing the lens itself.
Who benefits most
CLE may be recommended for patients who:
- Have presbyopia and require reading correction
- Have very high refractive errors
- Are not suitable candidates for laser vision correction
- May be at risk of developing cataracts later in life
Long-term vision correction advantages
Because the natural lens is replaced, CLE can provide long-term correction and also eliminates the possibility of future cataract development in the treated eye.
Comparing Procedures: Safety, Recovery, and Suitability
Each refractive surgery option has different advantages depending on the patient’s vision needs.
LASIK
- Suitable for many refractive errors
- Fast recovery
- Requires adequate corneal thickness
SMILE
- Minimally invasive with no corneal flap
- Often suitable for active individuals
- Typically used for myopia and astigmatism
Clear Lens Extraction
- Suitable for higher refractive errors or presbyopia
- Involves lens replacement rather than corneal reshaping
- May provide long-term correction for ageing eyes
When comparing procedures, doctors consider several factors:
- Age
- Lifestyle and occupation
- Eye health and corneal structure
- Long-term visual goals
Modern refractive surgery procedures generally have high safety and success rates when performed on appropriate candidates after thorough assessment.
How Candidacy Is Assessed
Before recommending refractive surgery, an ophthalmologist performs a comprehensive eye examination.
Comprehensive eye examination
This evaluation helps determine whether surgery is safe and suitable for your eyes.
Corneal thickness, eye health, and lifestyle evaluation
Several factors are assessed, including:
- Corneal thickness and shape
- Stability of vision prescription
- Presence of dry eye or other eye conditions
- Overall eye health
- Daily lifestyle and visual needs
Why not everyone is suitable for every procedure
Some patients may not be suitable candidates for certain procedures due to corneal structure, medical history, or existing eye conditions. In these cases, alternative treatment options may be recommended.
Next Steps: Consultation and Personalised Advice
Choosing refractive surgery is an important decision that should be based on professional guidance and a clear understanding of available options.
Importance of professional guidance
A qualified Singapore ophthalmologist can explain the benefits and limitations of each procedure and help determine which option aligns best with your vision needs.
Setting realistic expectations
While refractive surgery can significantly improve vision, it is important to have realistic expectations about outcomes, recovery time, and the possibility of future vision changes due to ageing.
Encouraging informed consultation
At International Eye Clinic, we conduct a detailed eye examination in Singapore to determine whether refractive surgery is suitable and which procedure may provide the best results for each patient. If you are considering vision correction surgery or would like to explore your options, arrange a consultation with us now.

For many people today, screens are an unavoidable part of daily life. From computers and tablets to smartphones and televisions, both work and leisure activities often involve prolonged screen use.
In Singapore, where many professionals spend long hours on computers and digital devices, complaints related to eye discomfort have become increasingly common. This has led to growing awareness of digital eye strain, a condition linked to extended screen exposure.
Understanding what digital eye strain is and how to manage it can help reduce discomfort and protect long-term eye health. Knowing when to go for an eye check-up in Singapore is also important to detect potential issues early and maintain clear, comfortable vision.
What Is Digital Eye Strain?
Digital eye strain refers to a group of vision and eye-related symptoms that occur after extended use of digital screens.
Definition and how it develops
Digital eye strain develops when the eyes work harder than usual to focus on screens for long periods. Unlike printed materials, digital displays can be harder for the eyes to process due to factors such as glare, pixelated text, and continuous scrolling.
This increased visual demand may lead to fatigue in the muscles responsible for focusing.
Difference between temporary strain and underlying eye issues
In many cases, digital eye strain is temporary and improves with rest. However, persistent symptoms may also indicate underlying problems such as uncorrected refractive errors, dry eye syndrome, or binocular vision issues.
A comprehensive eye examination can help determine whether symptoms are simply related to screen habits or caused by another eye condition.
Common Symptoms of Digital Eye Strain
Digital eye strain can present in several ways. Recognising these eye strain symptoms early can help prevent discomfort from worsening.
Tired, sore, or dry eyes
Prolonged screen use often leads to eye fatigue. The eyes may feel tired, irritated, or dry, especially after several hours of continuous work.
Blurred or fluctuating vision
Some people notice temporary blurred vision when looking away from the screen or difficulty refocusing between near and distant objects.
Headaches and eye discomfort
Visual strain can contribute to headaches, particularly around the temples or behind the eyes. This is often caused by prolonged focusing effort.
Neck and shoulder strain linked to screen use
Digital eye strain is often accompanied by physical discomfort. Poor posture or screen positioning may lead to neck, shoulder, and upper back strain.
Why Prolonged Screen Use Affects Vision
Several factors contribute to discomfort when using digital devices for long periods.
Reduced blinking and dry eyes
When focusing on screens, people tend to blink less frequently than normal. Reduced blinking can lead to faster tear evaporation, resulting in dry and irritated eyes.
Continuous near-focus and eye fatigue
Extended periods of close-up work require the eye’s focusing muscles to remain engaged for long periods. Over time, this can lead to fatigue and temporary vision fluctuations.
Poor posture and screen positioning
Improper workstation setup may force the eyes and neck into uncomfortable positions, increasing both visual and physical strain.
Practical Tips to Reduce Digital Eye Strain
Simple adjustments to daily habits and workstation setup can significantly reduce eye discomfort.
Follow the 20-20-20 rule
A widely recommended strategy is the 20-20-20 rule. Every 20 minutes, look at something at least 20 feet away for 20 seconds. This allows the eye muscles to relax.
Optimise screen distance and height
Your screen should ideally be positioned:
- About 50–70 cm from your eyes
- Slightly below eye level
This helps reduce strain on both the eyes and neck.
Adjust brightness, contrast, and font size
Make sure your screen brightness matches the surrounding lighting. Increasing text size and contrast can also make reading more comfortable.
Improve lighting and reduce glare
Avoid placing screens directly in front of bright windows or strong overhead lighting. Anti-glare filters or screen adjustments may help reduce reflections.
Maintain proper seating and workstation ergonomics
A comfortable workstation setup can prevent unnecessary strain. Ensure that:
- Your back is supported
- Feet rest flat on the floor
- The screen is aligned with your natural viewing angle
Daily Habits That Support Eye Comfort
Beyond workstation adjustments, certain daily habits can help maintain eye comfort.
Conscious blinking
Making a conscious effort to blink regularly can help maintain moisture on the surface of the eyes.
Taking regular breaks
Frequent breaks throughout the workday allow the eyes to relax and recover from prolonged focusing.
Staying hydrated
Adequate hydration helps support tear production, which keeps the eyes lubricated.
Limiting screen use before bedtime
Reducing screen exposure before sleep may help minimise eye fatigue and support better sleep quality.
When Digital Eye Strain Signals an Underlying Eye Issue
Although digital eye strain is common, persistent symptoms should not be ignored.
Persistent symptoms despite lifestyle changes
If discomfort continues despite taking breaks and adjusting screen habits, an eye examination may be necessary to identify underlying issues.
Vision changes that interfere with daily tasks
Blurred vision, difficulty focusing, or worsening headaches during screen use may indicate uncorrected refractive errors.
Increased headaches or discomfort
Frequent headaches or severe eye discomfort may also suggest the need for professional evaluation.
How an Eye Exam Can Help
An eye examination can help identify the root cause of digital eye strain and provide personalised solutions.
Identifying refractive errors
Conditions such as myopia, hyperopia, or astigmatism may contribute to visual strain when using screens.
Assessing dry eye or binocular vision issues
Your doctor may evaluate tear quality, eye alignment, and focusing ability to determine whether additional treatment is needed.
Tailoring solutions for screen-heavy lifestyles
Singapore Eye specialists can recommend strategies tailored to individuals who spend significant time using digital devices, including prescription lenses designed for computer work.
At International Eye Clinic, we provide comprehensive eye examinations to assess vision and address issues related to prolonged screen use. If you are experiencing ongoing eye strain or discomfort during screen use, book an appointment with us now.
FAQs
Can digital eye strain cause permanent eye damage?
Digital eye strain typically does not cause permanent eye damage, but prolonged discomfort may affect productivity and quality of life. Addressing symptoms early can help prevent ongoing strain.
Do blue light glasses help with digital eye strain?
Some people find that blue light filtering lenses reduce glare and improve visual comfort during prolonged screen use. However, maintaining proper screen habits and regular breaks remains the most effective way to reduce eye strain.
How many hours of screen time is considered excessive?
There is no strict limit, but spending several continuous hours without breaks may increase the risk of eye strain. Regular breaks and good screen habits are important for maintaining eye comfort.
Should children and teenagers be screened for digital eye strain?
Yes. Children and teenagers today often use digital devices for both school and recreation. If they experience symptoms such as headaches, eye rubbing, or blurred vision, an eye examination may be beneficial.
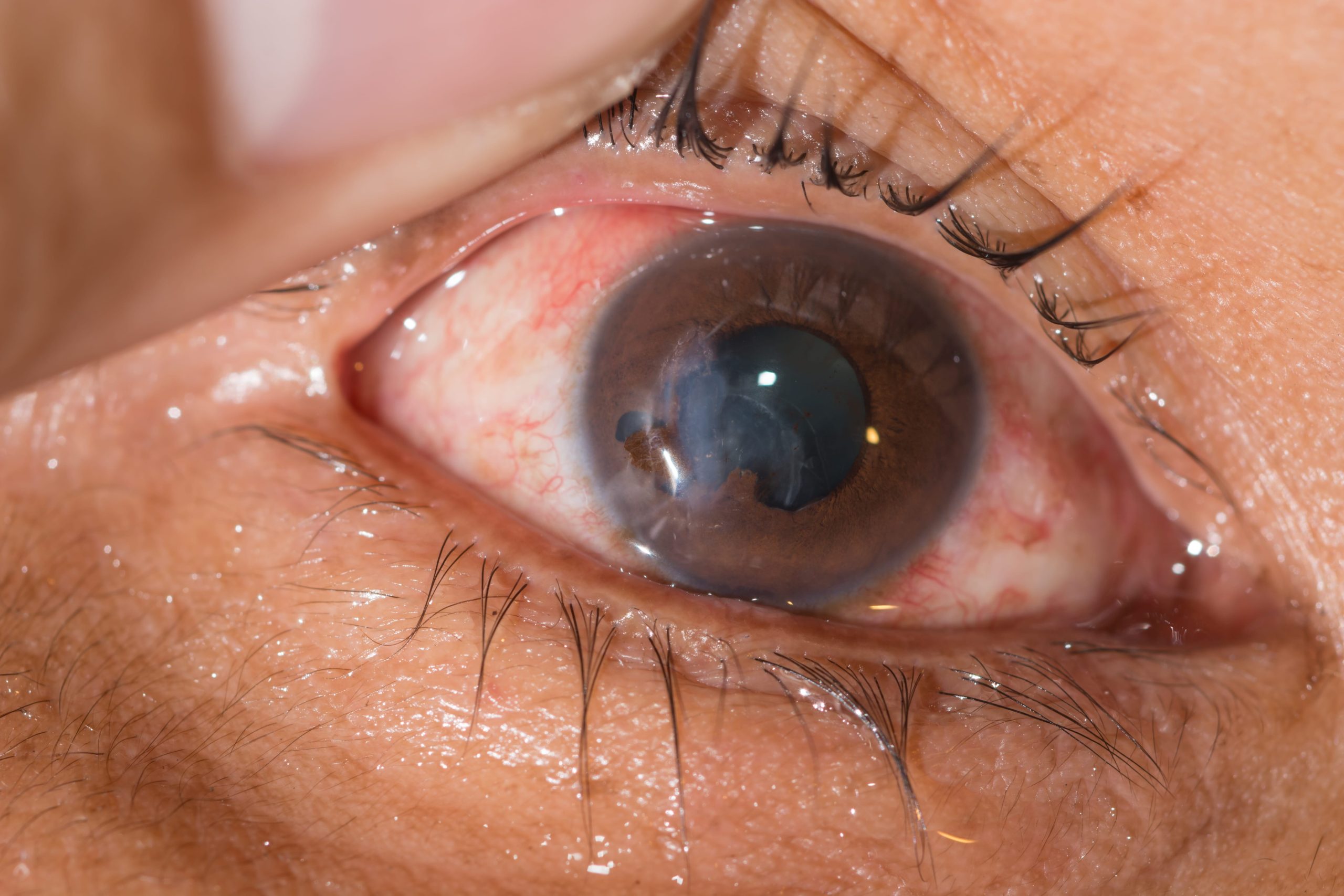
Glaucoma is often referred to as the “silent thief of sight” because it can damage vision gradually without obvious warning signs. By the time symptoms become noticeable, significant vision loss may already have occurred, making timely access to glaucoma treatment in Singapore critical for preserving eye health.
This condition affects the optic nerve, which is responsible for transmitting visual information from the eye to the brain. Once the optic nerve is damaged, the resulting vision loss is typically permanent and irreversible.
Many people are unaware they have glaucoma until the condition has progressed. This is why understanding the early signs of glaucoma and attending regular eye screenings is essential for protecting long-term vision.
What Is Glaucoma?
Glaucoma refers to a group of eye conditions that damage the optic nerve. This damage often occurs when the pressure inside the eye becomes too high, although glaucoma can also develop with normal eye pressure.
How glaucoma affects the optic nerve
The optic nerve is made up of thousands of nerve fibres that transmit visual signals to the brain. When glaucoma damages these fibres, parts of the visual field may gradually disappear.
Vision loss usually begins in the peripheral (side) vision, which is why many patients do not notice the problem in the early stages.
The role of eye pressure in vision loss
Inside the eye, a clear fluid continuously circulates to nourish internal structures. When this fluid does not drain properly, intraocular pressure (eye pressure) can increase.
Elevated eye pressure may place stress on the optic nerve, contributing to nerve damage over time. Managing eye pressure is therefore one of the key goals in glaucoma treatment.
Common Types of Glaucoma
There are several types of glaucoma, each affecting the eye in different ways.
Primary open-angle glaucoma
Primary open-angle glaucoma is the most common type of glaucoma. It develops slowly when the eye’s drainage system becomes less efficient, leading to a gradual increase in eye pressure.
Because the condition progresses slowly, many patients experience no noticeable symptoms in the early stages.
Angle-closure glaucoma
Angle-closure glaucoma occurs when the drainage angle inside the eye suddenly becomes blocked. This can cause a rapid rise in eye pressure and may lead to symptoms such as severe eye pain, headaches, blurred vision, and nausea.
This form of glaucoma requires urgent medical attention.
Secondary and less common forms
Other forms of glaucoma can occur due to underlying causes such as:
- Eye injury
- Inflammation inside the eye
- Certain medications
- Other eye conditions
Although less common, these forms can still lead to optic nerve damage if not properly managed.
Early Signs of Glaucoma
One of the challenges with glaucoma is that early-stage disease often causes few or no noticeable symptoms.
Why early-stage glaucoma often has no symptoms
In many cases, glaucoma initially affects the outer edges of the visual field rather than central vision. Because the brain compensates for these changes, patients may not realise that vision loss has already begun.
This is why routine eye examinations play a critical role in detecting the condition early.
Subtle warning signs patients may overlook
Although symptoms may be mild, some people may notice subtle changes, including:
- Gradual loss of peripheral vision
- Difficulty seeing clearly in low-light environments
- Frequent changes in glasses prescription
- Mild eye discomfort or pressure
- Seeing halos around lights
Recognising these glaucoma signs and symptoms early can help prompt timely evaluation.
Who Is at Higher Risk of Glaucoma?
While glaucoma can affect anyone, certain groups face a higher risk.
Age-related risk
The likelihood of developing glaucoma increases with age. People over the age of 40 are generally advised to undergo regular eye examinations to monitor for early changes.
Family history
Individuals with a family history of glaucoma are more likely to develop the condition themselves. If a close relative has glaucoma, regular screening becomes even more important.
Medical conditions
Certain health conditions may increase the risk of glaucoma, including:
- Diabetes
- High eye pressure
- Cardiovascular conditions
- Severe myopia (high short-sightedness)
Long-term steroid use
Long-term use of steroid medications, particularly steroid eye drops, may increase eye pressure and raise the risk of glaucoma.
Why Regular Eye Screening Is Critical
Because glaucoma often develops silently, routine eye screening is one of the most effective ways to detect the disease early.
How glaucoma can be detected before symptoms appear
An eye specialist in Singapore can identify early signs of glaucoma through several diagnostic tests. These tests evaluate eye pressure, optic nerve health, and changes in the visual field.
Detecting glaucoma early allows doctors to begin treatment before significant vision loss occurs.
Benefits of early diagnosis and monitoring
Early detection provides several advantages:
- Slowing or preventing further vision loss
- Allowing treatment before symptoms appear
- Monitoring disease progression more effectively
- Preserving long-term visual function
Recommended screening frequency by risk group
Screening frequency may vary depending on individual risk factors.
General recommendations include:
- Adults under 40: periodic eye checks every few years
- Adults over 40: regular eye examinations every 1–2 years
- Higher-risk individuals: more frequent screening as advised by an ophthalmologist
How Glaucoma Is Diagnosed During an Eye Exam
A comprehensive eye examination may include several tests to detect glaucoma.
Eye pressure measurement
Tonometry measures the pressure inside the eye and helps identify elevated intraocular pressure.
Optic nerve assessment
The doctor examines the optic nerve to check for structural changes or signs of damage.
Visual field testing
Visual field tests measure how well you can see objects in your peripheral vision. These tests can detect early vision loss caused by glaucoma.
Imaging scans
Advanced imaging technologies may be used to assess the optic nerve and retinal nerve fibre layer, allowing doctors to monitor subtle changes over time.
Living With Glaucoma: Long-Term Monitoring and Management
Although glaucoma cannot be reversed, it can often be managed effectively with early treatment and ongoing monitoring.
Importance of follow-up care
Patients diagnosed with glaucoma usually require long-term follow-up appointments to monitor eye pressure and optic nerve health.
Regular monitoring allows doctors to adjust treatment if necessary and reduce the risk of further damage.
Preventing progression through early intervention
Treatment options may include:
- Prescription eye drops
- Laser treatments
- Surgical procedures in certain cases
These treatments aim to lower eye pressure and protect the optic nerve.
When to Book a Glaucoma Screening
If you fall into a higher-risk group or notice changes in your vision, it is advisable to schedule an eye examination.
Symptoms that warrant immediate assessment
Seek professional evaluation if you experience:
- Sudden eye pain or headaches
- Blurred vision
- Halos around lights
- Rapid vision changes
- Nausea accompanied by eye discomfort
These symptoms could indicate a more urgent form of glaucoma.
Why specialist screening matters
Eye specialist clinics in Singapore like International Eye Clinic use advanced diagnostic equipment to detect early optic nerve changes and assess glaucoma risk accurately.
At International Eye Clinic, we provide comprehensive eye examinations and glaucoma screening to detect early signs of the condition and monitor long-term eye health. If you would like to schedule an eye check-up or learn more about Singapore glaucoma treatment, give us a visit.
FAQ
Can glaucoma be detected before vision loss occurs?
Yes. Glaucoma can often be detected before noticeable vision loss occurs through specialised eye tests that measure eye pressure, evaluate the optic nerve, and assess the visual field.
If I have no symptoms, do I still need screening?
Yes. Many patients with glaucoma have no symptoms in the early stages, which is why regular screening is important, especially for individuals over 40 or those with risk factors.
How often should I be screened for glaucoma?
Screening frequency depends on age and risk factors. Many adults benefit from eye examinations every 1–2 years, while higher-risk individuals may require more frequent monitoring.
Is glaucoma hereditary?
Yes. Glaucoma can run in families. If a close relative has been diagnosed with glaucoma, your risk may be higher, and regular screening is recommended.
Cataract surgery is a medical procedure used to remove a cloudy lens (called a cataract) from your eye and replace it with a clear artificial lens to restore vision.
One of the most common age-related eye conditions, cataract occur when the natural lens inside the eye becomes cloudy, causing vision to gradually become blurred or dim.
In a healthy eye, the lens is clear and helps focus light onto the retina. When cataracts develop, the lens becomes opaque, making it harder for light to pass through properly. As a result, everyday tasks such as reading, recognising faces, or driving at night may become more difficult.
Cataracts typically develop slowly over time. While glasses may temporarily improve vision in the early stages, surgery is often recommended once the cataract significantly affects daily activities.
Understanding the first signs of cataract and what cataract surgery involves can help patients feel more confident about seeking treatment.
Signs you may need cataract surgery
Eye cataracts usually develop gradually, so symptoms may be subtle at first. Many people initially attribute these changes to normal ageing.
Some of the signs of cataract include:
- Blurred or cloudy vision
- Increased sensitivity to light or glare
- Difficulty seeing at night
- Faded or yellowed colours
- Frequent changes in glasses prescription
- Seeing halos around lights
When these symptoms begin to interfere with daily tasks such as reading, driving, or using digital devices, it may be time to consider cataract surgery.
Who is a suitable candidate?
Cataract surgery is typically recommended when cataracts significantly affect vision and quality of life.
You may be a suitable candidate if:
- Your vision is no longer adequately corrected with glasses
- Daily activities such as driving or reading become difficult
- You experience persistent glare or halos from lights
- Cataracts interfere with the medical evaluation of other eye conditions
Cataract surgery is generally suitable for most patients, particularly older adults. However, an eye specialist will perform a thorough examination to confirm whether surgery is the appropriate option for your condition.
How modern cataract surgery works
Many patients ask, “What is cataract eye surgery?” In simple terms, the procedure involves removing the cloudy natural lens and replacing it with an artificial lens known as an intraocular lens (IOL).
Modern cataract eye surgery in Singapore is typically performed using phacoemulsification, a minimally invasive technique. During the procedure:
- A small incision is made in the eye.
- Ultrasound energy is used to break the cloudy lens into small fragments.
- The fragments are gently removed.
- A clear artificial lens is inserted to restore focusing ability.
The surgery is usually performed under local anaesthesia and does not require an overnight hospital stay.
Types of intraocular lenses (IOLs)
Intraocular lenses are artificial lenses designed to replace the eye’s natural lens after cataract removal.
Different types of IOLs are available, and the choice depends on your visual needs and lifestyle.
Common options include:
Monofocal lens
These lenses provide clear vision at one fixed distance, usually for distance vision. Glasses may still be needed for reading or close work.
Multifocal lens
Multifocal IOLs allow patients to see at multiple distances, which may reduce the need for glasses.
Toric lens
These lenses are designed for patients with astigmatism and help improve overall visual clarity.
Your ophthalmologist will recommend the most suitable lens option based on your eye health and visual preferences.
What to expect on surgery day
Cataract surgery is usually performed as a day procedure, meaning patients can return home on the same day.
Before the procedure, eye drops may be used to dilate the pupil and numb the eye. You will remain awake during the surgery, but the eye will be comfortably anaesthetised.
During the procedure:
- The surgery typically takes around 15 to 30 minutes
- You may notice bright lights but should not feel pain
- The surgical team will guide you through the process
After the procedure, your eye will be protected with a shield, and you will be given instructions on how to care for your eye during recovery.
Recovery timeline and post-surgery care
Most patients experience noticeable improvement in vision within a few days after surgery.
Typical post cataract surgery recovery includes:
First 24–48 hours
- Mild discomfort or a scratchy sensation may occur
- Vision may appear slightly blurry at first
- Protective eye shields may be recommended during sleep
First week
- Vision gradually becomes clearer
- Prescription eye drops help prevent infection and inflammation
- Avoid rubbing the eye or exposing it to water
First few weeks
- Normal daily activities can gradually resume
- Heavy lifting and strenuous exercise may need to be avoided temporarily
Your doctor will schedule follow-up appointments to monitor healing and ensure recovery is progressing well.
Long-term outcomes and vision improvement
Cataract surgery is one of the most commonly performed and successful eye procedures worldwide.
Many patients experience:
- Clearer and brighter vision
- Improved colour perception
- Reduced glare from lights
- Greater independence from glasses (depending on lens type)
Once the cloudy lens is removed, cataracts typically do not return. With appropriate care and regular eye examinations, most patients enjoy long-lasting visual improvement.
At International Eye Clinic, we provide detailed cataract assessments and modern cataract surgery to help restore clear vision. If you are experiencing symptoms or would like to explore cataract treatment Singapore options, you can learn more or arrange a consultation with us.
FAQs
Is cataract surgery safe?
Yes. Cataract surgery is widely regarded as a safe and effective procedure when performed by an experienced ophthalmologist. Serious complications are uncommon, and most patients recover well with improved vision.
How long does cataract surgery take?
The surgery itself usually takes 15 to 30 minutes, although you may spend a few hours at the clinic for preparation and post-procedure monitoring.
Will I still need glasses after surgery?
This depends on the type of intraocular lens used. Some patients may still require glasses for reading or close work, while others may experience reduced dependence on glasses.
When can I resume normal activities?
Most patients can return to light activities within a few days. However, strenuous exercise, swimming, and heavy lifting should generally be avoided for several weeks until the eye has fully healed. Your doctor will provide personalised guidance based on your recovery progress.

Vision problems are among the most common eye conditions affecting people today. In Singapore, refractive errors such as Myopia are particularly widespread due to a combination of genetics, lifestyle habits, and increased screen use.
Many people experience vision changes gradually. Because the symptoms develop slowly, they may be ignored or mistaken for simple eye strain or fatigue. However, untreated refractive errors can affect daily activities such as reading, driving, working on screens, and recognising faces at a distance.
Understanding the different types of eye conditions related to vision problems can help you recognise symptoms early and seek appropriate care.
What Are Refractive Errors?
Refractive errors are among the most common types of eye conditions affecting vision. They occur when the eye cannot properly focus light onto the retina, the light-sensitive layer at the back of the eye.
How light should focus in a healthy eye
In a healthy eye, incoming light passes through the cornea and lens and is focused precisely on the retina. This allows the brain to receive a clear image.
The cornea and lens work together to bend (refract) light so that objects appear sharp and well defined.
What happens when focusing is imperfect
When the shape of the eye or cornea prevents light from focusing correctly, images may appear blurred, distorted, or difficult to see at certain distances. These focusing issues are known as refractive errors.
The most common refractive errors include:
- Myopia (short-sightedness)
- Hyperopia (long-sightedness)
- Astigmatism
- Presbyopia
Each condition affects vision differently and may require specific treatment approaches.
Myopia (Short-Sightedness)
Myopia is one of the most common eye conditions in Singapore and across Asia. It occurs when distant objects appear blurry while nearby objects remain clear.
This happens when the eye is slightly longer than normal or when the cornea is too curved, causing light to focus in front of the retina.
Common causes and risk factors
Several factors may contribute to myopia:
- Genetic predisposition (family history)
- Excessive near work, such as reading or screen use
- Limited outdoor activity during childhood
- Rapid eye growth during school years
Myopia often develops during childhood and may worsen during adolescence before stabilising in adulthood.
Key symptoms
Common signs of myopia include:
- Blurry vision when looking at distant objects
- Squinting to see clearly
- Eye strain after visual tasks
- Frequent headaches
- Difficulty seeing road signs or classroom boards
Available treatment options
Treatment for myopia focuses on correcting how light enters the eye to improve visual clarity. Patients can explore suitable myopia treatment Singapore options based on their eye condition and lifestyle needs.
Glasses and contact lenses
Prescription glasses and contact lenses are the most common and straightforward solutions. They help refocus light correctly onto the retina, improving visual clarity.
Refractive surgery options
For suitable candidates, laser vision correction such as LASIK, EPI LASIK, SMILE, and SMILE Pro, may reduce or eliminate the need for glasses. Common procedures include:
- LASIK
- SMILE
- EPI-LASIK
These procedures reshape the cornea to improve how light focuses within the eye.
Hyperopia (Long-Sightedness)
Hyperopia occurs when nearby objects appear blurred while distant objects may remain clearer.
This happens when the eyeball is shorter than normal or when the cornea has insufficient curvature, causing light to focus behind the retina.
How hyperopia affects different age groups
Hyperopia can affect both children and adults. In children, mild hyperopia may sometimes go unnoticed because young eyes can compensate by adjusting focus.
In adults, the ability to compensate decreases with age, making symptoms more noticeable.
Common symptoms in children vs adults
Children may experience:
- Difficulty concentrating during reading
- Eye fatigue
- Frequent blinking or rubbing of the eyes
Adults may experience:
- Blurred vision when reading
- Eye strain during close work
- Headaches after prolonged visual tasks
Management and correction options
Hyperopia can be corrected with:
- Prescription glasses
- Contact lenses
- Refractive surgical procedures in appropriate cases
An eye specialist can recommend the most suitable option based on the severity of the condition and overall eye health.
Astigmatism
Astigmatism is another common refractive error caused by an irregular shape of the cornea or lens.
Instead of being perfectly round, the cornea may be shaped more like a rugby ball. This causes light to focus unevenly, leading to blurred or distorted vision.
Typical symptoms
People with astigmatism may experience:
- Blurred or distorted vision at all distances
- Difficulty seeing fine details
- Eye strain
- Headaches
- Squinting
Astigmatism often occurs alongside myopia or hyperopia.
Correction methods
Astigmatism can be corrected using:
- Specially designed toric glasses or contact lenses
- Laser vision correction procedures such as LASIK or SMILE
Treatment depends on the severity of the astigmatism and individual visual needs.
Presbyopia
Presbyopia is a natural age-related vision change that affects the eye’s ability to focus on close objects.
It typically develops after the age of 40 as the lens inside the eye gradually becomes less flexible.
Why does presbyopia develop with age
As we age, the natural lens of the eye stiffens and loses its ability to change shape easily. This makes it harder to focus on nearby objects such as books, mobile phones, or menus.
Presbyopia is not caused by disease but by the normal ageing process.
Early warning signs
Common early signs include:
- Difficulty reading small print
- Holding reading material farther away
- Eye strain during close work
- Needing brighter lighting when reading
Treatment solutions
Presbyopia can be managed with several solutions:
- Reading glasses
- Multifocal glasses or contact lenses
- Refractive surgery in selected patients
- Clear lens extraction, which replaces the natural lens with an artificial intraocular lens designed to improve vision at multiple distances
How Refractive Errors Are Diagnosed
Refractive errors are typically diagnosed through a comprehensive eye examination.
Eye tests used to identify each condition
Common diagnostic tests include:
- Visual acuity testing
- Refraction testing to determine lens prescription
- Corneal measurements
- Retinal and optic nerve evaluation
These tests help determine the exact cause of blurred vision and identify the type of refractive error present.
Why accurate diagnosis matters for treatment success
Accurate diagnosis ensures that the correct treatment is selected. Different refractive errors may require different correction methods, and some patients may benefit from surgical solutions while others may be better suited to glasses or contact lenses.
Choosing the Right Treatment Option
Treatment decisions are usually based on lifestyle needs, age, and the severity of the refractive error.
Glasses and contact lenses
For many patients, glasses and contact lenses remain the most convenient and effective way to correct refractive errors.
They provide immediate vision correction and can be easily updated as prescriptions change.
Refractive surgery
Some patients prefer a more permanent solution. Refractive procedures may include:
- LASIK
- SMILE
- Clear Lens Extraction
These procedures aim to improve the eye’s focusing ability by reshaping the cornea or replacing the natural lens.
Personalised treatment planning
Every patient’s eyes are different. An ophthalmologist will evaluate several factors before recommending treatment, including:
- Corneal thickness
- Overall eye health
- Lifestyle needs
- Age and stability of prescription
When to See an Ophthalmologist
While mild vision changes may seem manageable, certain symptoms should prompt a specialist consultation.
Red flags that require specialist assessment
You should see an ophthalmologist in Singapore if you experience:
- Sudden changes in vision
- Persistent eye strain or headaches
- Blurred vision that worsens over time
- Difficulty seeing clearly despite wearing glasses
- Visual distortion or double vision
Importance of regular eye examinations
Regular eye exams help detect vision problems early and ensure that treatment remains appropriate as your eyes change over time.
At International Eye Clinic, we provide detailed eye screening in Singapore to diagnose refractive errors and recommend suitable treatment options tailored to each patient. If you are experiencing changes in your vision or would like to explore modern vision correction options, you can learn more or book an appointment here.
FAQs
Can I have more than one refractive error?
Yes. It is common for people to have more than one refractive error. For example, someone may have both myopia and astigmatism, or develop presbyopia later in life while already having another condition.
Do refractive errors worsen over time?
Some refractive errors, particularly myopia, may worsen during childhood or teenage years before stabilising in adulthood. Presbyopia naturally progresses with age.
Are refractive surgeries permanent?
Refractive surgery results are generally long-lasting, but natural ageing changes in the eye may still occur over time. Your ophthalmologist can explain expected outcomes based on your condition.
At what age should vision changes be checked?
Vision changes should be evaluated at any age. Children with suspected vision issues should undergo early assessment, while adults should seek evaluation if they notice persistent blurred vision, eye strain, or difficulty focusing.
Many eye conditions develop slowly and may not cause noticeable symptoms in the early stages. By the time vision changes become obvious, the condition may already be more advanced. This is why regular eye check-ups are an important part of maintaining long-term eye health.
A comprehensive eye exam allows an eye specialist to evaluate your vision and check for signs of common eye conditions such as glaucoma, cataracts, or retinal diseases. These examinations are especially important for people with risk factors such as ageing, diabetes, high myopia, or a family history of eye disease.
For many patients, the idea of visiting an eye specialist in Singapore can feel unfamiliar or even slightly intimidating. Understanding what happens during the exam can help you feel more prepared and reassured before your appointment.
What is a comprehensive eye exam?
A comprehensive eye exam is a detailed assessment of your overall eye health and vision. Unlike a basic vision screening, which usually checks only how well you can see, a comprehensive exam evaluates multiple aspects of your eyes.
During the visit, an ophthalmologist or eye specialist will assess:
- Your visual clarity and prescription
- The health of the retina and optic nerve
- Your eye pressure
- The structures at the front of the eye
- Any early signs of eye disease
The goal is not only to determine whether you need glasses or contact lenses, but also to detect potential eye problems early before they affect your vision.
Step-by-step: Tests performed during an eye exam
A comprehensive eye exam usually involves several tests. Each test examines a different aspect of your eye health.
Vision testing
Vision testing measures how clearly you can see at different distances.
You may be asked to read letters on a chart to assess your visual acuity. This helps determine whether you have refractive errors, such as:
- Myopia (short-sightedness)
- Hyperopia (long-sightedness)
- Astigmatism
If needed, the doctor may perform a refraction test to determine the correct prescription for glasses or contact lenses.
Eye pressure (glaucoma screening)
Eye pressure testing helps screen for glaucoma, a condition that can damage the optic nerve if left untreated.
The test, called tonometry, measures the pressure inside your eye. In many clinics, this may be done using a quick puff of air or a gentle instrument that briefly touches the surface of the eye after numbing drops are applied.
The procedure is fast and typically causes minimal discomfort.
Retinal and optic nerve assessment
Your doctor will also examine the retina and optic nerve, which are critical for vision.
This part of the exam helps detect conditions such as:
- Diabetic retinopathy
- Macular degeneration
- Retinal tears or detachments
- Glaucoma-related optic nerve damage
Special imaging tests or retinal photographs may be taken to allow a detailed view of the back of the eye. In some cases, eye drops may be used to dilate the pupils, allowing a clearer examination of the retina.
How long does the exam take?
A comprehensive eye exam typically takes about 20 to 40 minutes, depending on the tests required.
If additional imaging or specialised tests are needed, the appointment may take slightly longer. Your doctor will explain each step during the process so you know what is being done and why.
If pupil dilation is required, your vision may remain blurry for a few hours afterwards, so you may wish to avoid driving immediately after the appointment.
What conditions can be detected early?
A comprehensive eye exam can detect many eye conditions before symptoms appear.
Some of the common conditions that may be identified include:
- Glaucoma
- Cataracts
- Age-related macular degeneration (AMD)
- Diabetic eye disease
- Retinal problems
- Dry eye syndrome
Early detection allows treatment to begin sooner, which can help preserve vision and prevent complications.
In some cases, eye exams may also reveal signs of broader health issues such as diabetes or high blood pressure, as changes in blood vessels can sometimes be seen in the retina.
How often should you get your eyes checked?
The recommended frequency for eye examinations depends on your age, health, and risk factors.
General guidelines include:
- Adults under 40: every 2–3 years if there are no symptoms
- Adults 40–60: every 1–2 years
- Adults above 60: yearly eye examinations are often recommended
People with certain conditions may require more frequent monitoring, including those with:
- Diabetes
- High myopia
- Glaucoma or a family history of glaucoma
- Previous eye surgery
- Existing eye diseases
Your eye specialist can advise on a schedule that is appropriate for yo
When to book an eye exam at a specialist clinic
If you experience any changes in your vision or eye discomfort, it is advisable to consult an eye specialist promptly. Symptoms that should not be ignored include:
- Blurred or distorted vision
- Frequent headaches related to eye strain
- Sudden flashes of light or floaters
- Eye pain or redness
- Difficulty seeing at night
Even if you feel your vision is normal, regular eye examinations remain important for preventive care.
At International Eye Clinic, we provide comprehensive eye examination Singapore services to assess both vision and overall eye health. Our team uses modern diagnostic equipment to detect potential issues early and guide patients on appropriate treatment options.
If you would like to schedule an eye check-up or learn more about our services, visit our clinic website here.
FAQs
Is a comprehensive eye exam painful?
A comprehensive eye exam is generally not painful. Most tests are quick and non-invasive. Some procedures may involve mild discomfort, such as bright lights or brief eye drops, but these sensations usually last only a short time.
Can eye exams detect systemic health conditions?
Yes. Eye examinations can sometimes reveal signs of systemic health issues such as diabetes, hypertension, or high cholesterol, as these conditions may affect the blood vessels in the retina.
Do I need an eye exam if I have no symptoms?
Yes. Many eye diseases develop without noticeable symptoms in the early stages. Regular eye examinations allow eye specialists to detect problems early, when treatment is often most effective.
The decision you are about to make is one of the most important of your vision journey. For many, cataract surgery is viewed as a necessary medical procedure to address a decline in vision. While this is true, it is also a remarkable and unique opportunity—a chance to redefine how you see the world for the rest of your life. The clouding of your natural lens has brought you to this point, but the path forward is filled with choices that can correct not only the cataract but also lifelong vision issues like nearsightedness, farsightedness, and astigmatism.
The purpose of this guide is to serve as your comprehensive, unbiased partner in understanding these choices. The world of intraocular lenses, or IOLs, can seem complex, filled with technical terms and competing claims. My goal here is to demystify this technology, to provide you with the clear, in-depth knowledge you need to have a meaningful and productive conversation with your surgeon. Together, we will explore your unique visual goals and how they align with the incredible advancements in modern ophthalmology.
It is essential to understand a fundamental truth from the outset: there is no single “best” lens for everyone. The concept of a universally superior IOL is a myth. Instead, there is only the lens that is best for you. This choice is a deeply personal one, a careful balance of what is technologically possible and what is personally important—a reflection of your lifestyle, your profession, your hobbies, and even your personality. This guide will empower you to navigate that decision with confidence.
The Standard Choice: Understanding Monofocal IOLs
How They Work
The monofocal IOL is the most common and time-tested type of lens implanted today. Its design philosophy is one of elegant simplicity and optical purity. It has a single, fixed point of focus. When light enters the eye, the lens bends it to one precise focal point on the retina. Before surgery, you and your surgeon will decide where you want this single point of focus to be set. The vast majority of patients choose to have their monofocal lenses set for excellent distance vision, which is useful for activities like driving or watching television
The Pros:
- Excellent Clarity and Contrast: Monofocal lenses are known for providing exceptionally sharp and clear vision at their designated focal point.
- Time-Tested and Predictable: Having been used for decades, the outcomes with monofocal lenses are highly predictable and reliable.
- Typically Covered by Insurance: In most cases, the cost of a standard monofocal IOL is covered by national health insurance and most private insurers.
- Lower Incidence of Glare and Halos: Compared to more advanced lenses, patients with monofocal IOLs tend to experience fewer visual disturbances like glare and halos around lights, especially at night.
The Cons:
- Dependence on Glasses: The primary drawback of a monofocal IOL is the need for glasses for other distances. If your lens is set for distance vision, you will require reading glasses for near tasks like reading a book or using a smartphone.
Lifestyle Profile: Who is a Good Candidate for Monofocal IOLs?
Monofocal IOLs are an excellent choice for individuals who:
- Do not mind wearing glasses for certain activities.
- Prioritize the absolute sharpest quality of vision at a single distance.
- Have a budget as a primary consideration.
The Freedom of Choice: Exploring Multifocal IOLs
How They Work
The multifocal IOL is designed with a different philosophy: to provide a broad range of vision and reduce dependence on glasses. It achieves this through a more complex optical design. Most modern multifocal IOLs are based on a principle called diffractive optics. The surface of the lens is engineered with a series of microscopic, concentric rings, similar to the grooves on a vinyl record. These rings act to split the incoming light, simultaneously directing it to two or three distinct focal points on the retina. A bifocal lens creates points for distance and near, while a trifocal lens adds a third point for intermediate vision (at arm’s length). Your brain then performs a remarkable feat of neuroadaptation, learning to pay attention to the clearest, most relevant image for the task at hand while suppressing the others.
The Pros:
- Significant Reduction in the Need for Glasses: The principal advantage of multifocal IOLs is the high degree of spectacle independence they offer. Many patients find they no longer need glasses for the majority of their daily activities.
- Clear Vision at Multiple Distances: These lenses are designed to provide clear vision for a wide range of tasks, from reading a menu to seeing a sign down the street.
The Cons:
- Potential for Glare, Halos, or Starbursts: The design that allows for multiple focal points can also cause light to scatter, leading to visual phenomena like glare, halos, or starbursts, particularly noticeable at night.
- Possible Reduction in Contrast Sensitivity: Some patients may experience a slight decrease in the ability to distinguish between subtle shades of color or objects in low light.
- Premium Lens with Out-of-Pocket Costs: Multifocal IOLs are considered a premium option and typically involve additional costs not covered by standard insurance.
- Neuroadaptation: Your brain will need time to learn how to process the new visual information from the multiple focal points, a process known as neuroadaptation.
Lifestyle Profile: Who Thrives with Multifocal IOLs?
Multifocal IOLs are often best for individuals who:
- Have a strong desire to be free from glasses for most of their daily tasks.
- Lead active lifestyles that involve frequent switching between near, intermediate, and far vision.
- Are willing to adapt to a new way of seeing and are not significantly bothered by the potential for night vision disturbances.
The Modern Hybrid: A Closer Look at EDOF IOLs (Extended Depth of Focus)
How They Work
The Extended Depth-of-Focus (EDOF) IOL represents a third philosophy, born directly from the desire to provide an extended range of vision while minimizing the known side effects of multifocal technology. Unlike multifocal lenses that split light into multiple discrete points, EDOF lenses employ a different and more subtle optical strategy. They use sophisticated technologies, such as precisely manipulating an optical property called spherical aberration or using non-diffractive wavefront-shaping designs, to create a single, elongated focal point. This elongated focus creates a continuous and seamless range of clear vision that stretches from distance through to intermediate (arm’s length) ranges, without the “gaps” in vision that can occur with some multifocal designs
The Pros:
- Excellent Distance and Intermediate Vision: EDOF lenses are particularly well-suited for our modern, screen-oriented world, providing sharp vision for tasks like using a computer, tablet, or seeing the dashboard of a car.
- Lower Risk of Glare and Halos: Compared to multifocal lenses, EDOF IOLs generally have a lower incidence of visual side effects like glare and halos.
- A More “Natural” Range of Vision: Many patients report that the transition between different distances feels smoother and more natural with EDOF lenses.
The Cons:
- Near Vision May Not Be as Sharp: While excellent for intermediate tasks, the near vision with EDOF lenses might not be as crisp as that provided by multifocal lenses. You may still need reading glasses for fine print or prolonged up-close work.
- Premium Lens with Associated Costs: Like multifocal lenses, EDOF IOLs are a premium option and come with out-of-pocket expenses.
Lifestyle Profile: Who is an Ideal Candidate for EDOF IOLs?
EDOF lenses are an excellent match for individuals who:
- Spend a significant amount of time on computers or other intermediate-vision activities.
- Desire a broader range of vision than monofocal lenses but are concerned about the potential side effects of multifocal lenses.
- Are comfortable with the possibility of needing reading glasses for very fine, up-close tasks.
A Side-by-Side Comparison: Making the Right Choice for You

Lifestyle Scenarios
- The Avid Reader and Hobbyist: A multifocal lens may be ideal for its strong near vision, eliminating the need for reading glasses during close-up work.
- The Frequent Driver (Day and Night): A monofocal lens offers the crispest distance vision with the lowest risk of halos, making it an excellent choice. An EDOF lens is also a strong contender due to its lower risk of night vision issues compared to a multifocal.
- The Working Professional: An EDOF lens excels here, providing clear distance vision for presentations and sharp intermediate vision for computer work, reducing the need for glasses at a desk.
- The Active and Social Individual: A multifocal or EDOF lens offers the freedom from glasses that allows for spontaneous activities like reading a menu, playing sports, or shopping without visual interruption.
Important Considerations and Next Steps
The best way to begin narrowing down these options is to reflect on your own life, priorities, and personality. The following questions are designed to help you prepare for the conversation with your surgeon. There are no right or wrong answers, only honest ones that will guide you to the best choice for you.
Your Daily Life and Vocation
- What are the most common visual tasks in your day? Do you spend hours driving, working on a computer, or looking at a car dashboard? An affirmative answer here places a high value on intermediate vision, a key strength of the EDOF IOL.
- What does your profession demand? Are you an artist, a photographer, a pilot, or a commercial truck driver who requires the absolute sharpest, highest-contrast vision, especially in challenging light or at night? These professions often prioritize the pristine visual quality and low risk of dysphotopsia offered by a Monofocal IOL.
- What are your most cherished hobbies? Are they primarily close-up activities like reading, sewing, model-building, or fly-tying? This highlights a strong need for excellent near vision, which is a primary benefit of Multifocal IOLs, or can be achieved with a near-set Monofocal IOL.
Your Relationship with Glasses
- On a scale of 1 to 10, how much do you dislike wearing glasses? Is achieving spectacle independence a primary motivation for you in pursuing this surgery? A very high score on this question suggests that a premium lens like a Multifocal or EDOF IOL would be a worthwhile consideration to achieve greater visual freedom.
- Imagine your life after surgery. Would you be comfortable reaching for a pair of low-power reading glasses for certain tasks like reading a medicine bottle, or is your goal to eliminate glasses from your life entirely? Being comfortable with occasional readers makes you an excellent candidate for an EDOF lens. A desire for total freedom from glasses points more strongly toward a Multifocal lens
Your Personal Tolerance and Personality
- How sensitive are you to glare from headlights when you drive at night? If you already find night glare to be very bothersome, this should serve as a significant point of caution against Multifocal IOLs, which are known to increase these phenomena.
- How would you describe your personality? Are you a perfectionist who notices and is bothered by small visual imperfections? Or are you generally more adaptable, flexible, and easy-going? A perfectionistic tendency often aligns well with the clean, predictable, and artifact-free optics of a Monofocal IOL. A high degree of adaptability is a key trait for success and satisfaction with a Multifocal IOL.
Your Ocular Health and Budget
- Do you have any other underlying eye conditions? A history of glaucoma, age-related macular degeneration (AMD), epiretinal membrane, or even significant chronic dry eye can impact the final choice. These conditions can compromise visual quality on their own, and the complex optics of Multifocal or EDOF lenses can sometimes exacerbate these issues. In many such cases, the crisp, high-contrast vision of a Monofocal IOL is the safest and most appropriate choice.
- What is your budget for this procedure? It is important to be aware that while the cataract surgery itself and the implantation of a standard Monofocal IOL are typically covered by Medicare and private insurance, Multifocal and EDOF lenses are considered premium or “lifestyle” upgrades. As such, they involve a significant out-of-pocket expense that is not covered by insurance. This should be viewed as an investment in a specific visual lifestyle.
Partnering for Your Best Vision
We have journeyed through the science of vision, the mechanics of cataracts, and the sophisticated philosophies behind the three major categories of intraocular lenses. The central message, I hope, is clear: the concept of a single “best” IOL is a myth. The true goal of this process is to find the optimal match between the unique, intricate tapestry of your life and the specific technological profile of a lens.
This guide is intended to be the first step in your decision-making process—to arm you with knowledge, clarify the trade-offs, and help you articulate your personal priorities. The second, and most crucial, step is the detailed consultation with your ophthalmologist. It is in this partnership—combining your self-knowledge and visual goals with your surgeon’s deep expertise and comprehensive evaluation of your eyes—that the final, personalized recommendation is co-created.
Cataract surgery today is more than a restorative procedure; it is a transformative one. You stand at the threshold of a new, clearer future, with an opportunity to see the world in a way that is customized for you. I look forward to taking that final step with you and helping you achieve your best possible vision.
Choosing an eye specialist is one of the most important healthcare decisions you can make for yourself or your family. Whether you’re experiencing new symptoms, managing a chronic condition, or seeking care for a loved one, the process can feel overwhelming. From scheduling a routine eye examination in Singapore to finding treatment for more complex issues, how do you choose the right professional among so many qualified options?
This guide is designed to provide a clear, objective, and step-by-step framework to help you make an informed decision with confidence. The “right” specialist is not about finding a name on a list; it’s about finding a medical partner whose expertise aligns with your specific condition and whose approach to care makes you feel respected and understood.
Understanding Key Eye Care Professionals in Singapore
First, it’s helpful to understand the different roles within eye care to ensure you are seeking the correct type of professional for your needs.
- Ophthalmologist: An ophthalmologist is a medical doctor (MD) who has completed extensive medical and surgical training to specialise in all aspects of eye care. They are qualified to diagnose and treat the full spectrum of eye diseases, perform complex eye surgery for conditions like cataracts and glaucoma, and prescribe medication. If you have a medical eye condition, require surgery, or need a comprehensive medical eye examination, an ophthalmologist is the specialist you should see.
- Optometrist: An optometrist is a primary eye care provider who performs eye examinations, tests for vision problems, and prescribes corrective lenses like glasses and contact lenses. They can also diagnose and manage some medical eye conditions.
- Optician: An optician is a technician trained to design, verify, and fit eyeglass lenses and frames based on a prescription provided by an ophthalmologist or optometrist.
Step 1: Verify Credentials and Qualifications
This is the foundational, non-negotiable step in choosing any medical specialist in Singapore. Verifying a doctor’s credentials ensures they have met the rigorous standards required to practice medicine and their chosen specialty.
Check the Singapore Medical Council (SMC) Register
Every medical doctor practicing in Singapore must be registered with the Singapore Medical Council (SMC). This is the first and most important check you should perform. The SMC maintains a public, searchable professional register. You can use this official resource to confirm that your potential doctor is registered and holds a valid practicing certificate.
Look for Specialist Accreditation
Beyond basic medical registration, you should ensure the doctor is a registered specialist in ophthalmology. In Singapore, the Specialists Accreditation Board oversees the formal recognition of medical specialists. A doctor listed on the Register of Specialists has completed years of advanced, formal postgraduate training in ophthalmology and has passed rigorous specialist examinations.
Consider Sub-specialty Fellowship Training
Many of Singapore’s leading ophthalmologists pursue further sub-specialty training, known as a fellowship, after completing their specialist accreditation. This often involves spending one to two years at a world-renowned international institution, focusing on a specific area like glaucoma, retinal diseases, or pediatric ophthalmology. A fellowship is a strong indicator of a doctor’s deep expertise and commitment to a particular field of eye care. When reviewing a doctor’s profile, look for mentions of fellowship training, as this demonstrates a higher level of specialised skill.
Step 2: Align the Specialist’s Expertise with Your Condition
Ophthalmology is a broad field with many sub-specialties. Just as you would see a cardiologist for a heart condition, aligning your specific eye issue with a doctor’s sub-specialty is crucial for receiving the most appropriate care.
Here are some clear examples of when to seek a specific sub-specialist:
- Cataracts: While many ophthalmologists perform cataract surgery in Singapore, you may want to look for a surgeon who has a high volume of experience and is proficient in using advanced technologies and a wide range of modern intraocular lenses (IOLs).
- Glaucoma: This is a chronic condition that requires long-term management. A glaucoma specialist will have in-depth knowledge of the latest diagnostic tools, medications, lasers, and surgical options, including Minimally Invasive Glaucoma Surgery (MIGS).
- Retinal Issues (e.g., AMD, Diabetic Retinopathy): Conditions affecting the retina require the care of a retinal specialist. They are experts in managing complex issues like age-related macular degeneration (AMD), diabetic eye disease, and retinal detachments.
- Children’s Eye Conditions (e.g., Myopia, Squints): A child’s eyes are still developing, and their conditions require specialised care. A pediatric ophthalmologist is trained to diagnose and manage issues like childhood myopia, amblyopia (lazy eye), and strabismus (squints) in a child-friendly environment.
Step 3: Prepare a Checklist of Questions for Your Consultation
Your first consultation is a critical opportunity to gather information and assess if the doctor is the right fit for you. Being prepared with a list of questions can empower you to have a productive discussion.
Here is a practical checklist of essential questions to ask your potential eye specialist :
On Experience & Qualifications:
- “What are your qualifications, and where did you complete your sub-specialty fellowship training?” This helps you understand their specific training and expertise.
- “How many procedures like mine do you perform annually?” A surgeon who performs a high volume of a specific surgery is likely to be highly proficient and adept at handling potential challenges.
On Your Diagnosis:
- “Could you explain my condition and what the test results mean in simple terms?” A good doctor should be able to communicate complex information clearly, ensuring you fully understand your diagnosis.
On Treatment Options:
- “What are all the available treatment options for my condition?” This ensures you are aware of all possibilities, not just one.
- “What technology do you use for this surgery, and why is it the most appropriate for my case?” This question helps you understand if the clinic uses modern equipment and how it benefits you directly.
- “What are the pros and cons of the different intraocular lenses (IOLs) for my lifestyle?” (For cataract surgery). This is a crucial question to ensure the outcome matches your visual goals.
On Risks and Complications:
- “What are the potential risks of this procedure, and how do you manage complications if they occur?” A responsible surgeon will be transparent about risks, however rare, and have a clear plan for managing them.
On Costs:
- “Can you provide a detailed, itemised breakdown of all costs involved?” A reputable clinic should provide clear financial counselling, including the surgeon’s fees, facility charges, and any follow-up costs, to avoid surprises.
Step 4: Evaluate the Clinic and Overall Patient Experience
Beyond the doctor’s individual credentials, the clinic environment and its approach to care play a significant role in your overall experience.
- Patient-Centric Communication: A good specialist and their team will take the time to listen to your concerns, answer your questions thoroughly, and involve you in the decision-making process. You should feel like a partner in your own healthcare.
- Use of Technology: A clinic equipped with a comprehensive range of modern diagnostic and surgical tools can often provide more accurate diagnoses and effective treatments. Look for information on the technology they use on their website or ask about it during your visit.
- Financial Transparency: The clinic should be upfront and clear about all costs. A reputable practice will provide a detailed financial estimate before any procedure, helping you understand what to expect.
- Insurance Compatibility: Before your appointment, it is wise to check if the clinic is on your insurance provider’s panel. This can help minimise your out-of-pocket expenses. You can typically do this by contacting your insurance provider or the clinic’s administrative staff.
Conclusion
Choosing an eye specialist in Singapore is a significant decision that deserves careful consideration. By following a structured approach—verifying credentials, matching the sub-specialty to your needs, asking detailed questions, and evaluating the overall patient experience—you can confidently select a qualified ophthalmologist who is the right fit for you. This partnership is key to protecting your vision and ensuring your long-term eye health.
Choosing the right eye specialist is a partnership in your health. Our ophthalmologist is committed to these principles of transparency and patient-focused care. To learn more about her credentials and experience, we invite you to view her profile here.

If you’re considering LASIK surgery in Singapore, you’re likely looking forward to tossing your glasses for good—and waking up to sharp, unaided vision. But you may also be wondering: What does recovery actually feel like? Will it hurt? How long before life feels normal again? And of course, how do you care for your eyes in a place like Singapore, where the mix of air-conditioning and humidity can be a bit tricky?
Having walked hundreds of patients through this journey, I can tell you that good recovery isn’t just possible—it’s the norm. Let me guide you through what to expect, how to heal well, and what real recovery looks like, from Day 1 to the moment you forget you ever had poor eyesight.
LASIK isn’t just effective—it’s one of the most trusted elective procedures in Singapore. Over 98% of patients in Singapore report satisfaction with their LASIK results within the first 6 months of recovery.
What Happens Right After LASIK Surgery
Immediately after LASIK, most patients describe feeling mild irritation—as if an eyelash got stuck in the eye. That’s normal. You may also experience:
- Blurry or hazy vision
- Light sensitivity
- Excessive tearing
- Mild burning or stinging sensation
You’ll need someone to bring you home, wear your eye shield as instructed, and rest your eyes for the remainder of the day. Avoid phones, screens, and reading—even if you feel fine. Your cornea needs this downtime to begin healing properly.
LASIK Recovery Timeline: Day-by-Day Breakdown
Here’s what a typical recovery looks like:

What to Avoid After LASIK Surgery
Avoiding complications is all about what not to do. Here’s your post-LASIK Do-Not list:
- No rubbing your eyes
- No swimming (pools or sea) for 2–4 weeks
- No eye makeup for 1 week
- No strenuous exercise or heavy lifting for 1 week
- Avoid dusty, smoky, or windy environments
Instead:
- Use protective eye shields at night
- Keep up with prescribed eye drops
- Wear UV-protective sunglasses outdoors
How to Speed Up Your LASIK Recovery
Your eyes are healing—but you can help the process:
- Stay hydrated. Dry eyes can delay recovery.
- Follow your medication schedule. Don’t skip lubricating drops.
- Limit screen time. The less strain, the faster the healing.
- Attend all follow-up appointments. We check for healing progress and subtle complications.
- Invest in good sunglasses. HealthHub SG notes that UV exposure can slow healing.
Differences Between LASIK and Epi-LASIK Recovery
At eyedoctor.com.sg, we offer multiple options to suit different eyes and lifestyles—including LASIK, Epi-LASIK, and SMILE Pro. Here’s how they compare, especially in terms of recovery:

SMILE Pro is the latest evolution in refractive surgery. It uses a small keyhole incision to remove a lenticule inside the cornea, without creating a flap. This reduces discomfort, speeds up recovery, and helps maintain corneal strength and shape—making it especially suitable for patients with active lifestyles or dry eyes.
Visit LASIK/EPI-LASIK/SMILE Pro page to learn more about SMILE Pro Treatment
Warning Signs to Watch For
Call your clinic immediately if you notice:
- Severe pain or vision loss
- Redness that worsens instead of fading
- Pus or unusual discharge
- Flashes of light or sudden floaters
Remember, complications are rare—but acting early makes all the difference
LASIK Recovery FAQs:
- How long does it take to fully recover from LASIK in Singapore?
Most patients achieve full clarity within 1 month; some take up to 3–6 months for night vision adjustments. - Can I go back to work after LASIK?
Yes—usually after 2–3 days, depending on your work environment (avoid screens if possible). - What foods or supplements help with LASIK recovery?
Omega-3s and Vitamin A (from oily fish, leafy greens) support eye health. - Is Epi-LASIK recovery longer than traditional LASIK?
Yes, due to surface healing; expect more downtime and discomfort. - When can I wear makeup or eye products again?
After 1 week, and only if your surgeon clears it. - Can I exercise after LASIK?
Light exercise after 3–5 days; avoid contact sports for a few weeks. - Is it normal to have blurry vision days after LASIK?
Yes, especially in the first week. Use lubricants and rest. - When should I schedule my follow-up appointment?
Usually within 24–48 hours, then 1 week, 1 month, 3 months, and 6 months. - How is LASIK recovery in Singapore different?
Singapore’s humidity can cause extra tearing or foggy glasses pre-op. Post-op, air-conditioned spaces may dry eyes—carry lubricants with you.
Whether you’re weighing your options or already booked for surgery, understanding the LASIK recovery process helps you take charge of your eye health.
Ready to improve your vision safely and permanently?
Book a consultation at **eyedoctor.com.sg today, where our experienced specialists offer LASIK, Epi-LASIK, and SMILE Pro—the latest advancement in minimally invasive, bladeless vision correction. With cutting-edge technology, faster recovery times, and a focus on long-term eye health, we tailor every treatment to your lifestyle. Take the first step toward clearer vision today.
Let’s make clear vision your new normal.


